 Crew Weunski (ESTEEM '21)
Crew Weunski (ESTEEM '21)
Throughout our lives, we are predisposed to experiencing pain. 1.5 to 2 billion people are affected by pain worldwide each day. Pain can take many forms, such as in joints or the spine, and varies in its degree of severity. For those that have chronic conditions, they will seek a pain management specialist for treatment.
Pain management specialists perform various procedures, but many involve injecting anti-inflammatory drugs/steroids directly to the pain source. The use of imaging is varied among physicians and procedures. They will use different techniques (such as x-ray fluoroscopy or ultrasound) to ensure they are injecting the medication or placing a needle at the correct location, without causing damage to the surrounding critical structures.
Each imaging method has drawbacks that can have either long-term effects on the physician or can result in needle misplacement (and thus ineffective pain relief for the patient). The primary imaging modality for many pain management procedures is x-ray fluoroscopy, which exposes both the patient and physician to harmful radiation. Long-term exposure to ionizing radiation may increase the risk of developing malignant cancer for physicians. Fluoroscopy is a more costly imaging modality than ultrasound. It is two-dimensional, grayscale, and requires contrast enhancement injection for proper visualization. Since physicians use a two-dimensional imaging technique for an inherently three-dimensional problem, they must interpolate the 2D data into a 3D space using knowledge of anatomy and experience.
Ultrasound is a cheaper solution that does not rely on potentially harmful x-ray radiation. Ultrasound allows a physician to see the anatomy in real-time and does not utilize any contrast enhancement injection. On the other hand, ultrasound is also two-dimensional and grayscale and is highly operator dependent. There is a high learning curve for physicians to be comfortable using this imaging modality. Thus, there is a high skill level required for the successful placement of a needle under ultrasound.
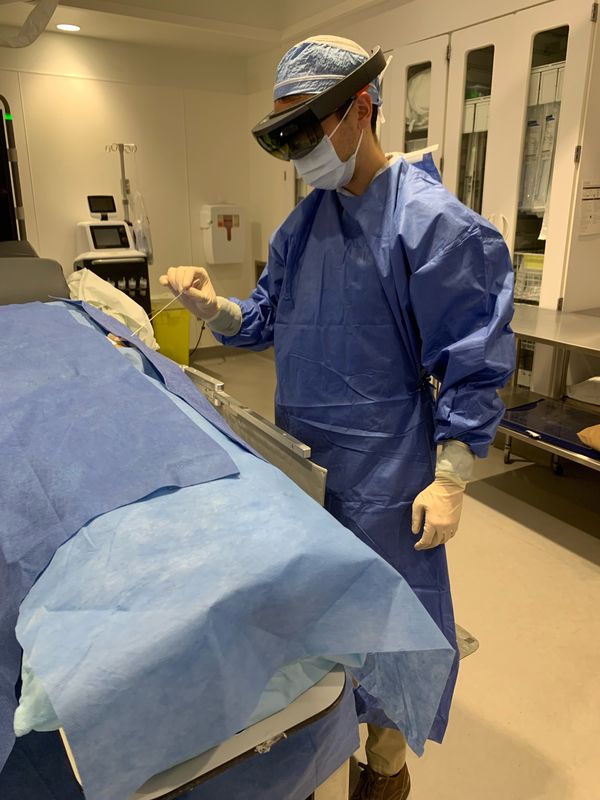
To overcome these challenges, MediView XR is developing MediScout™: a point-of-care ultrasound system that uses augmented reality and spatial computing to enable physicians to directly live stream an ultrasound feed and project it as a digital image (“hologram”) within the operator’s view. The system allows users to collaborate with and learn from other experienced remote physicians in real-time, which will decrease complications and increase procedural confidence. MediView is currently evaluating potential use cases for MediScout™. As such, I am interviewing pain management physicians to understand better how and if this technology could help their procedures. I will be developing recommendations based on detailed market research and validation interviews with pain management physicians, and developing a go-to-market strategy for this technology.
I am very excited to be working on this project with MediView XR. They have a great team from various technical and business backgrounds that are all extremely passionate about bringing augmented reality technology to physicians around the nation. I am looking forward to the remainder of this project with MediView!